Most people give little or no thought to medical errors in their daily lives. Unless you have actually been affected by a medical error, the possibility that it could happen to you probably seems fairly far-fetched. But is it?
We take a look at medical errors, their causes, and what, if anything, can be done about them.
Top Health Statistics
- Medical billing errors cost Americans $210,000,000,000 annually.
- Roughly 12,000,000 Americans are misdiagnosed each year.
- Medical errors cause an estimated 250,000 deaths in the United States annually.
- As many as 80 percent of medical bills contain at least one error.
- A little more than 4,000 surgical errors occur each year.
- It’s estimated that 7,000 to 9,000 patients die every year from medication errors.
As you can see from our top stats, medical errors are abundant in the American health care system. What qualifies as a medical error, and how can you know if you or a loved one has been the victim of one?
What Is a “Medical Error”?
According to the book Medical Error, it is defined as a “preventable adverse effect of medical care, whether or not it is evident or harmful to the patient.” (Emphasis added.)
As a patient, you may not even know a medical error has taken place, and even if you do know about it, the medical error may not negatively affect you in any way. However, many medical errors are quite serious, and can even result in death.
According to data provided by the U.S. Department of Health and Human Services, one in seven patients on Medicare in a hospital setting is the victim of a medical error.
A Johns Hopkins study released in 2016 estimated that roughly 250,000 people die annually because of medical errors. That would make medical errors the third leading cause of death in the United States, behind only heart disease and cancer.
Top Ten Causes of Death in the United States (2016)
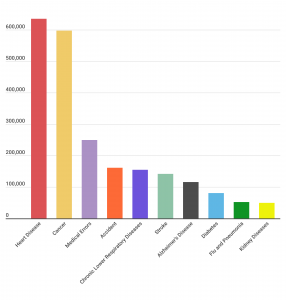
*It should be noted that the annual death rate from medical errors is an extrapolation based on a smaller pool of data.
As you can see from the chart above, heart disease and cancer each kill roughly 600,000 Americans per year. They are followed by medical errors, then accidents at 161,000 deaths per year.
Some studies indicate that death from medical errors could be even higher due to the way medical errors are reported on death certificates—with as many as 440,000 people dying every year from medical errors. The number of deaths caused by medical errors is far too high.
High-Risk Medical Errors
Sometimes, a medical error poses little physical risk to a patient, such as getting billed for a procedure that didn’t take place.
Other times, the consequences are life or death—and those types of high-risk medical errors typically occur in fast-paced, high-pressure environments, such as hospital emergency rooms, hospital intensive care units, and operating rooms in hospitals.
But that doesn’t mean medical errors can’t happen at your care provider’s office or other outpatient settings.
Types of Medical Errors
Now that we’ve defined what counts as a medical error, what are the most common types of medical errors in the United States?
- Misdiagnosis
- Billing errors
- Incorrect medication/incorrect dosage
- Incorrectly identifying a patient
- Surgical errors
We explore each type of error in more detail below.
Misdiagnosis
Misdiagnosis occurs when a patient with one illness or disease is told they have a different illness or disease. According to a 2014 study, roughly 12,000,000 Americans are misdiagnosed at outpatient facilities every year.
The study’s authors concluded that this issue creates a “substantial patient safety risk” and should be addressed. Reducing the chance of patient harm should be a main priority.
Of the 12,000,000 total Americans receiving a misdiagnosis, roughly 50 percent could be seriously harmed by getting the wrong diagnosis, as shown in the chart below.
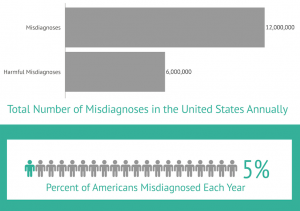
That total number breaks down to about 5 percent of the adult U.S. population.
According to a study that analyzed more than 300 medical claims between 2007 and 2013, the following health issues were the most commonly misdiagnosed.
- Stroke
- Heart attack
- Spinal epidural abscess
- Pulmonary embolism
- Necrotizing fasciitis
- Meningitis
- Testicular torsion
- Subarachnoid hemorrhage
- Septicemia
- Lung cancer
- Fractures
- Appendicitis
Some of these may not sound very familiar dressed up in their medical terminology, so they are described here in everyday terms.
A spinal epidural abscess is infected fluid and germs on the spinal cord, and it can be deadly. It is harder to diagnose because two of the main symptoms (fever and back pain) are vague and could be caused by many non-fatal diseases or illnesses.
Pulmonary embolisms are more commonly referred to as a blood clot in one or both lungs. These can be deadly if not diagnosed and treated in time. In fact, roughly one-third of all people who have this condition and have not been diagnosed or treated will die.
This condition is also tough to diagnose if someone already has heart or lung disease.
Necrotizing fasciitis is a fast-spreading bacterial infection. According to the Centers for Disease Control and Prevention, time is of the essence when diagnosing and treating this disease to minimize loss of tissue and prevent death.
However, as many as one-third of people who contract this disease will still die, even with treatment.
Meningitis is a bacterial infection that affects the brain and spinal cord. It can be easily misdiagnosed since the symptoms match up nearly identically with the flu. This, too, can be a deadly disease if not treated quickly.
Testicular torsion occurs when blood flow is cut off to the testicle because a blood vessel becomes twisted. If caught within six hours, there’s a high likelihood the testicle can be saved. Otherwise, the testicle will need to be removed. Take a look at the time-sensitive nature of testicular torsion:
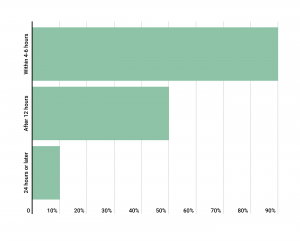
As you can see from the chart above, if testicular torsion is treated within six hours, there’s a 90 percent chance the testicle can be saved. After 24 hours, that rate drops to only 10 percent.
Subarachnoid hemorrhages are also known as bleeding on the brain, and have several causes, including concussions and traumatic brain injuries. This condition can also be deadly if not caught in time.
Septicemia, also known as blood poisoning, occurs when bacteria enters the bloodstream.
If you think you’re suffering from any of these health issues, but you can’t find a health care provider to take you seriously, keep pushing until someone does the necessary testing to rule out or confirm any potential issues. It just may be your life on the line.
Billing Errors
Billing errors happen when patients are charged for procedures they did not receive, or are charged for staying longer at an in-patient facility than they actually did, or correct procedures/stays have been coded incorrectly due to data entry errors.
In fact, medical billing errors cost Americans around $210 billion annually.
Most medical bills, around 80 percent of them, contain some type of error, and the errors are rarely in favor of the patient. According to one report, there are around 70,000 diagnosis codes that could be used, and around 71,000 procedure codes available. That makes errors nearly inevitable.
Medication Errors
Another major medical error that affects public health in the United States is incorrect medications or dosages of those medications. It costs over $40 billion per year to care for and treat patients who were victims of medication errors.
In the United States, between 7,000 and 9,000 patients die from medication errors every year.
The types of errors that fall under this category include:
- Prescribing the wrong medication.
- Failing to include a necessary part of the prescription.
- Telling the patient to take the prescription at the wrong time of day.
- Giving the improper dose of medication.
- Failing to check whether the patient is allergic to that medication.
- Failing to check whether there are other medications the patient takes that could interact with the prescribed drug.
- Transcribing the prescription incorrectly.
In hospitals or outpatient facilities performing surgical procedures, this can also include anesthesia errors—either using too much or too little, or using an anesthetic the patient is allergic to.
Patient Misidentification
Believe it or not, incorrect identification of patients occurs frequently enough to make this list. You may think it wouldn’t be possible to confuse which patient is having which procedure performed, or even which patient the doctor is there to see, but it happens.
In the chart below, we examine a few instances related to frequency of misidentification.
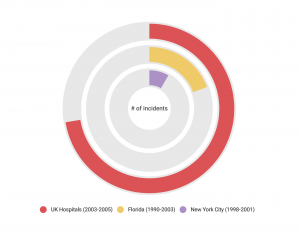
Between 2003 and 2005, hospitals in the United Kingdom reported 236 incidents or near-incidents in which patients were misidentified.
Florida practitioners indicated that between 1990 and 2003, the wrong patient had gotten surgical procedures in 67 cases.
And in New York City, over a three-year span, the wrong patient had gotten an invasive medical procedure in 27 cases.
In one incident from Boston, a patient with healthy kidneys was mistaken for a patient with a kidney tumor. The healthy patient’s kidney was removed—and the error was only discovered after the surgery had been performed.
The following graphic provides summary numbers from several misidentification incidents across the United States.

It’s difficult to know exactly how many cases of misidentification occur nationwide, but most researchers believe actual instances are much higher than reported numbers, and the impact on the affected individuals is enormous.
Surgical Errors
Finally, we take a look at surgical errors. According to data from 2012, surgical errors resulted in $1.3 billion in medical malpractice payouts annually. The annual number of surgical errors rose above 4,000, and were nearly all preventable.
In fact the authors of the study this data is based on called the surgical errors “never events,” which means the errors never should have happened in the first place. These include things like leaving a surgical tool inside the patient, or operating on the wrong limb.
The graphic below goes into more detail on common surgical errors and their frequency.

Are these surgical errors harmful, though? According to the data below—yes!
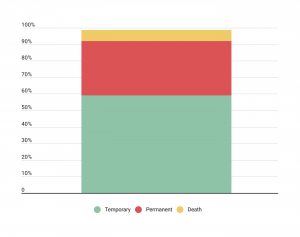
While the majority of surgical errors only resulted in temporary injuries (59 percent), nearly 40 percent of these errors resulted in permanent injuries or death. Less than two percent of surgical errors resulted in no injury.
And most of the surgeons who committed surgical errors (two-thirds) had been involved in at least two prior medical malpractice actions.
What Causes Medical Errors?
What are the factors that go into creating a medical error, and are they fixable? Can we reduce the number of medical errors, and more importantly, the adverse effects of these errors on patients?
We review a few of the most typical components that, in combination or alone, cause the vast majority of medical errors in the United States.
- Lack of training
- Assigning tasks to inappropriate staff
- Rare or copy-cat illnesses
- Lack of adequate testing
- Time-sensitivity—the treatment or procedure must be done immediately
- Complexity of the illness or health issue being treated
- Age of the patient
- New procedures
Let’s look a little more closely at each of the factors listed above.
Training
In some cases, errors are caused by new staff, who are still learning or haven’t encountered a specific situation before, and therefore haven’t had the necessary training to know how to handle the issue presented.
Inappropriate Assignments
Other times, errors are due to assigning tasks to the wrong staff. For example, one study found that pharmacy technicians were making medical formulations instead of the pharmacists, who were specially trained and educated for that purpose.
Rare Illness
Sometimes, a patient may have a rare illness. Because these illnesses are rare, they’re often misdiagnosed as something else, especially if their symptoms mimic another, much better known disease or illness. For example, meningitis and the flu have nearly identical symptoms.
Testing
Unfortunately, a patient’s pre-existing health condition may limit the amount of diagnostic testing that’s done to determine the cause of reported symptoms.
In some cases, heart attacks in female patients may be dismissed as simply an extreme panic attack, because the heart attack symptoms women experience are almost identical to those of panic attacks, and further testing may not be done.
Lack of adequate testing also affects obese patients, as it was found that not all necessary diagnostic testing was done for these patients, leading to diagnostic errors or failure to diagnose any illness or disease at all.
Patients with pre-existing mental health disorders were especially vulnerable to this. For example, if a patient with depression reports a sudden lack of energy, they may be prescribed a higher dose of their antidepressant, instead of being tested for thyroid function or other possible culprits.
Time Pressure
And any time there is pressure to get a diagnosis completed right away, or a procedure done immediately, there is a greater risk of missing the actual cause of the symptoms or performing the procedure incorrectly. (Or performing the incorrect procedure.)
Complexity
The more complex an illness or disease is, or the more complex the treatment protocol required to help the patient, the higher the risk that something will get missed along the way.
Age
Patients at both the high and low ends of the age spectrum are often victims of medical errors, as well. The youngest members of the population can’t articulate their symptoms or what has been helpful in alleviating those symptoms, and that is often the same for the oldest members of the population.
New Procedures
Finally, if a new procedure is developed for the treatment of a disease or illness, there is always a learning curve related to putting that new procedure successfully into practice. Sometimes a health care provider picks up the new procedure quickly; but if they don’t, medical errors may occur.
How Can You Protect Yourself?
At this point, you may be wondering how you can protect yourself and your loved ones from these types of errors. There are several things you can do, so take heart. All of these factors will contribute to your well-being.
- Ask questions at every stage. When seeking a diagnosis, ask your doctor about specific tests you’d like to have done, or about specific health concerns you have. If you’re scheduled for surgery, ask questions about the specific procedure, or about any medications you may be prescribed.
- Get a second opinion. While it may feel awkward or like you’re betraying your doctor’s trust in some way, it’s in your best interests to get a second opinion when it comes to difficult diagnoses or major treatment options.
- Do your homework. Research your condition and the appropriate treatment options as much as possible before any surgery or medications have been prescribed. The better informed you are, the easier it will be to determine if your treatment plan is correct and the best option for your situation.
- Request an itemized bill. This way you can check dates of service, services provided, and the doctors involved in your treatment and/or diagnosis. Any medical mistakes will be much easier to identify than if you receive a summarized statement.
- Bring someone with you. Two heads are better than one! It’s nerve-wracking to be in a doctor’s office or hospital and having someone you trust at your side can make it easier to ask questions and share pertinent information.
National Academy of Medicine
The National Academy of Medicine, formerly known as the Institute of Medicine, is a non-profit organization that was originally created to provide leadership in the field of healthcare.
Two of their publications, Crossing the Quality Chasm (2001) and To Err is Human: Building a Safer Health System (1999) shone a light on medical errors at the beginning of the 21st Century and garnered national attention.
Today, they continue to issue publications related to the state of America’s health care system, as well as examining health care issues world-wide.
Where Can I Learn More?
To get more information on specific health conditions, the Mayo Clinic’s website has a “condition finder” where you can type in any condition and see what information they have on it. You can also look through an A-Z directory of conditions.
The Centers for Disease Control and Prevention also lists multiple conditions, research being done, and the latest treatments for certain diseases.
Condition-specific organizations, such as the American Heart Association, are great options for getting more information on a specific condition you may be concerned about.
The Agency for Health Care Research and Quality’s website has resources to help patients advocate for themselves and includes things patients can do to help prevent medical errors, such as asking hospital staff if they’ve washed their hands before they touch anything that will touch you (needles, catheters, food trays, your skin).
You can always report a doctor or surgeon to your state’s medical board if you have concerns about how they have handled your condition.
In Summary…
Getting proper medical care is necessary for your health and safety. While none of us want to believe that medical errors will happen to us, based on the frequency of these issues, it’s highly probable that you will experience at least one of the errors outlined here during your lifetime.
Educate yourself and your loved ones as well as you can on your specific health issues or health concerns, and don’t be afraid to push back if something doesn’t seem right. That persistence might just save your life.
Sources
- CNBC, “The Third-Leading Cause of Death in U.S. Most Doctors Don’t Want You to Know About.”
- The National Center for Biotechnology Information, “Medical Error.”
- Johns Hopkins Medicine, “Study Suggests Medical Errors Now Third Leading Cause of Death in the U.S.”
- Agency for Healthcare Research and Quality, “20 Tips to Help Prevent Medical Errors Patient Fact Sheet.”
- Centers for Disease Control and Prevention, “FastStats: Leading Causes of Death.”
- MedicalNewsToday, “1 in 20 American Adults ‘Misdiagnosed in Outpatient Clinics Each Year’.”
- MedicineNet, “Definition of Cerebrovascular Accident.”
- Wikipedia, “Myocardial Infarction.”
- Medline Plus, “Epidural Abscess.”
- The National Center for Biotechnology Information, “Spinal Epidural Abscess: Common Symptoms of an Emergency Condition.”
- Mayo Clinic, “Pulmonary Embolism.”
- The Centers for Disease Control and Prevention, “Necrotizing Fasciitis: All You Need to Know.”
- Mayo Clinic, “Meningitis.”
- TeensHealth from Nemours, “Testicular Torsion.”
- Mayfield Brain & Spine, “Subarachnoid Hemorrhage and Vasospasm.”
- Healthline, “Septicemia.”
- Anxiety and Depression Association of America, “Am I Having a Panic Attack or a Heart Attack?”
- Healthline, “Up to 80% of Hospital Bills Have Errors. Are You Being Overcharged?”
- Becker Hospital Review, “Medical Billing Errors Growing, Says Medical Billing Advocates of America.”
- The National Center for Biotechnology Information, “Medication Errors.”
- Agency for Healthcare Research and Quality, “Mistaken Identity.”
- ECRI Institute, “Patient Identification Errors.”
- JAMA Network, “Wrong-Site and Wrong-Patient Procedures in the Universal Protocol Era.”
- Boston Globe, “14 Instances of Right Procedure, Wrong Patient in Mass.”
- WebMD, “Thousands of Mistakes Made in Surgery Every Year.”
- National Academy of Medicine, “To Err is Human: Building a Safer Health System.”
- National Academy of Medicine, “Crossing the Quality Chasm: A New Health System for the 21st Century.”
